Dr. Joanne Magro “The Power of the Stiletto.” News Column (05)
(Published: 2025/06/26 at 1:06 pm)
Edition Five- Week Five; News Column:
Written by: Dr. Joanne Magro

Dr. Joanne Magro: The OPIOID Epidemic (Part Two)
Dr. Joanne Magro and Her Experience in The Field Working the Emergency-Room
“As the exponential rise in fatalities from opiates was bombarding our ERs, it was completely demoralizing for our physicians and staff as the patients were young. They had their whole life ahead of them. When listening to many stories through their loved ones, it was unconscionable to just sit back and ride the wave. Mind you, almost all overdoses that results in death were unintentional as Fentanyl began to infiltrate the market on all fronts.
Fentanyl being found in what these patients was thought to be heroine, Adderall, a stimulant used to treat ADHD as well as being used recreationally. You name it…FENTANYL was the name of the game…everyday people were playing Russian Roulette as they were
buying their arsenal on the streets which much of was laced. Almost every day we were pronouncing someone DOA…Dead on Arrival despite our field workers administering the reversal agent known as Narcan. Some of my worst overdose cases involved my own nurse’s children who were working that same shift. How does a ship that I’m at the helm of recover from incidents like this. We still have 40 plus patients waiting to be seen; however, we lost one of our own. The Emergency Department is a bonified mess as this snapshot in time was something straight out of the movies. Basically, time stood still. There’s no way to just go back to our daily duties even though our ship was drowning much akin to the Titanic to say the least. We let our staff a momentary time to grieve and support each other as much as we could. But these were times that left an imprint on all of us. A grieving mother, lunging into the trauma room shaking their dead son and screaming. These were not favorable times for any of us on that shift that day. Most people think of us as characters on ER TV shows. Well, my friends, we are not actors and actresses, we are “The Real Deal”. Emergency Rooms seem somewhat glamorous to the outside world, let me tell you from firsthand experience, this is not a TV show, it is not a glamorous job, but we do our best…you win some and you lose some…and onto the next patient you go as if nothing ever happened.”
Dr. Joanne Magro explains to us the details regarding this ongoing epidemic. This written piece is labeled as part two of the informative news series.
Tackling the War on Drugs
Nationwide, communities face an unprecedented rise in substance misuse fatalities. Close to 100,000 deaths occur each year in the United States which involve opioids. To stem the tide of this crisis, some communities are doubling down on the war on drugs, despite clear evidence that increasing arrests and incarceration does not lower drug use.
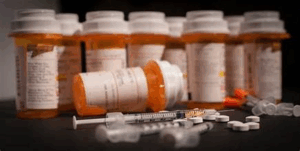
But an increasing number of cities are bucking the trend and adopting models that treat substance misuse as a disease, not a crime. Instead of criminalizing substance use disorders, communities are focusing on saving lives and reducing the harmful effects of drug use.
“Cities must develop inclusive approaches that treat all substance use disorders as a disease, not a crime.”
The idea of “harm reduction” may seem like commonsense today, but it signifies a radical departure from traditional U.S. responses to drug use, which relied heavily on the criminal justice system. More and more cities are expanding access to clean syringes, launching safe-injection facilities, and decriminalizing possession of controlled substances. Public acceptance of these approaches was unthinkable a few years ago. Today, however, they are filtering into the mainstream. In fact, support for harm reduction spans the ideological spectrum. These strategies are underway in red and blue states alike, representing promising steps toward dismantling the country’s failed drug policy agendas.
The War on Drugs and Harm Reduction
The rise of public support for harm reduction strategies cannot be separated from the fact that white Americans have been hit the hardest by the opioid epidemic, though black communities are increasingly experiencing its effects. Today, more and more Americans are acknowledging the failure of the war on drugs. Drug courts were an important first step away from the status quo. As the name implies, however, they are still part of the criminal justice system, and participants who do not successfully complete the program could face lengthy sentences of incarceration. More than 3,100 jurisdictions (which is a low-ball
number) have established drug courts, which pair intensive recovery services and case management with rigorous accountability mechanisms for participants. This movement touts the model as a more effective and cost-efficient alternative to the “revolving door” of recidivism. “Unless you address the underlying issue of addiction, which is what drug courts do, then you’re likely to offend.” There is a robust debate about how to reduce the punitive aspects of drug courts, but today, policymakers and the public alike are increasingly adopting approaches that treat substance misuse as a health issue rather than a criminal justice one.
Syringe Access Programs
Syringe access programs are one example of harm reduction programming that has gained traction over the past years. Sometimes referred to needle exchanges, syringe access services provide people with sterile injection equipment to reduce the incidence of syringe sharing- a risky practice linked to transmission of bloodborne infections. By ensuring that
people have access to clean injection equipment; these programs can significantly reduce the incidence of new HIV and Hepatitis C diagnoses. In Wahington DC, for example, a syringe access program reduced new HIV cases by 70 percent over two years, saving the city an estimated $44.3 million in averted healthcare costs. About 20 years ago, syringe access was so controversial that the U.S Congress banned the use of federal funds to support these programs, pending an evaluation of their efficacy.
Today syringe access programs currently operate in most states. The rapid adoption of the syringe access model is a testament to its success at improving health outcomes. I can go on and on about the adoption of some new programs that are emerging, however, the bottom line is that we need more Federal funding, more access to mental health facilities and practitioners, more Community based Outreach Programs, easier access for
those people in rural areas, more case managers to help people to navigate through the system which is a n extremely daunting task. Basically…we need more of everything and that starts at the TOP of the food chain per se and then the trickle-down effect will have remarkable outcomes. We cannot stigmatize people who have a “disease” just as we treat high blood pressure or diabetes with using old verbiage like junkies, addicts. We need to
engage with them and be able to offer a safe and efficacious plan for their recovery as well as their re-entry back into a sober world.
Safe-Injection facilities
Numbers of U.S. cities are taking harm reduction one step further by adopting a strategy known as supervised injection facilities (SIFs). Sometimes called ‘safe-injection sites” or “supervised consumption facilities,”. These sites are staffed by medical professionals who
are trained to recognize and respond to fatal dosages, mitigating the risks associated with substance misuse. Like syringe access services, SIF’s offer sterile injection equipment and safe disposal options for used needles. Furthermore, SIFs are an avenue to treatment as people build vital connections with health care providers who are on hand to provide
immediate referrals to social services and treatment options.

Other Effective Strategies
Naloxone
Naloxone is a lifesaving drug that reverses the symptoms of opioid overdose. By expanding access to naloxone, communities nationwide are preventing unnecessary overdose fatalities. Distributing Naloxone to lay people-particularly the families and friends of individuals at high risk of overdose-has also proven to effective at preventing fatalities.
Additionally, many syringe access sites offer free naloxone kits and overdose education programming for clients and their loved ones.
Conclusion
In a departure from the failed policies of the war on drugs, local leaders are now rallying around strategies that reduce the harm of substance misuse. Gripped by the devastation of the opioid crisis, cities are bringing once-fringe policy solutions into the mainstream, citing their successful track records at saving lives and preventing disease. The strategies that are
detailed in this column represent promising progress toward ending decade old policy agenda of criminalizing substance misuse. Cities must develop inclusive approaches that treat all substance use disorders-not just opioid misuse as a disease…NOT A CRIME!!!
Stay tuned for the third series as we hit the streets and obtain in real time the life of individuals with substance abuse disorder.
“The Doctor Joanne Magro Foundation for Physician Health and Wellness”/ jmagromd@gmail.com and Peer Support Specialist for Addiction Recovery and Support Community Outreach/ jmagromd@gmail.com.
—————————
What topics would you like to read next by authorship of Dr. Joanne Magro in the upcoming edition of her column? Leave your comments below!
ManualMagazines.com
This website uses cookies to provide you with the best browsing experience.
One Comment
Bijal Vohra
I enjoyed reading every word of this, the war on drugs is SO REAL and you eloquently targeted the problem/solution and bravely identified what’s NOT working – Bravo Joanne- for your constant courage, extensive research and effort for your cause, and your resilience to continue saving lives even while you’re not in the ER.